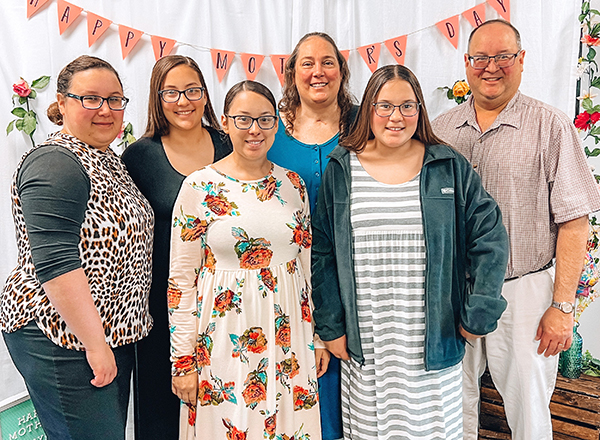In Her Own Words
Salazar Thankful for FHN’s Breadth of Care
‘A Hysterectomy … and a Whole Lot More’
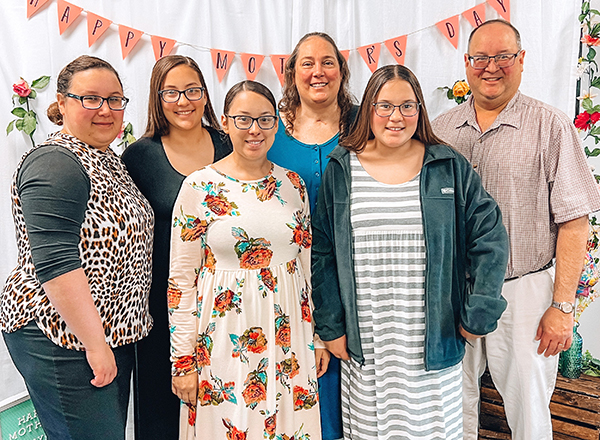
Tamara is thrilled to enjoy special moments with her family, like this Mother’s Day event with her daughters and husband. Pictured left to right are Sarah (who became a CNA after caring for her mom); Rachel; Ashley; Tamara; Hannah; and Ray.
In 2018, FHN’s Women’s Health Team confirmed Tamara Salazar needed a hysterectomy due to a prolapsed uterus. It was regularly causing her discomfort, but wasn’t an emergency. She put it off to help another family member who was ill, and then COVID-19 came … with a vengeance.
Busy with life – work, her husband, and four active girls – Tamara thought she could fend off COVID-19 with some time off and a few days in bed. “I can beat it,” she said. Instead, she wound up in the hospital and ended up in a coma. “My blood oxygen went down to 49 percent and they didn’t think I was going to make it,” she shares. She spent 94 days away from home, finally waking on Thanksgiving Day, 2021.
Luckily, thanks to “an amazing group of compassionate professionals” from FHN (see sidebar on page 3) and beyond, Tamara survived her COVID-19 ordeal. She considers herself about 80 percent of the way back to a healthy life. But, almost five years later, she still needed that hysterectomy – and now she had complications to consider.
Complications Make Surgery a Challenge
Her bout with COVID-19 compromised Tamara’s lungs, and her primary care physician, Rebecca Pedersen, MD, was concerned about her going under anesthesia. Yet, her prolapsed uterus was worse than before and causing more problems. Heavy blood flow during menstrual cycles made it impossible for Tamara to leave home, even for her post-COVID physical therapy, and she had also developed a hernia near her belly button that needed attention.
Dr. Pedersen suggested that both surgeries be done consecutively to minimize anesthesia time, and encouraged a pre-op review by Ob/Gyn physician Dr. Lee Sesslar, who agreed with the recommendations, and her pulmonologist, Dr. Mohamed Zeater*, who teams with FHN. He approved the surgery, but encouraged the briefest anesthesia time possible under the lowest amounts necessary for proper sedation.
Enter: Two Talented Surgeons
To help plan Tamara’s surgery, Ob/Gyn physician and surgeon Keith Martin, MD, FACOG, and surgeon Javeria Qureshi, MD, MPH, FACS, worked with anesthesiologist Maria Laporta, MD*, to decide how to best optimize and expedite the procedures.
Each physician consulted with Tamara and went out of their way to keep her informed and educated. Dr. Martin handled Tamara’s hysterectomy first, followed by Dr. Qureshi, who repaired the hernia. Both surgeries went as planned, and Tamara was in and out of the operating room quickly and without problems. “Both my surgeons had amazing bedside manners. They never hurried me and were so kind and concerned.”
At her post-op check with Dr. Martin, he confirmed that everything had healed well and the surgery was a success.
“Dr. Martin was such a cheerleader,” says Tamara. “He is so personable and immediately put me at ease. He assured me that everything had healed well, and I felt so blessed to be under his skilled care.” All the problems she was experiencing from her prolapsed uterus and hernia are gone.
‘They Went Above and Beyond’
Even though Tamara is not quite back to 100 percent after her long journey, she is keenly aware of her progress and grateful for each day she feels stronger and better. “Last week I climbed three flights of stairs at Meet the Teacher night for my high school senior, and I struggled, but I did it,” she declares.
“It is all about the little things – I can feed myself, I can roll over in bed, I can do the laundry, and now I am looking forward to all my children’s big moments that I might have missed. I appreciate each minute with my kids and am grateful to God for not only my immediate family, but my FHN family.
They all put me first. They helped me not only with their medical expertise and follow through, but also with their compassion, kindness, and encouragement. These people went above and beyond to make me better. I trust FHN more than any other facility and I 120 percent recommend them to anyone.”